 |
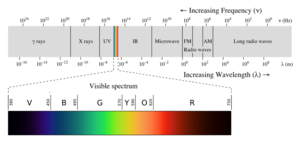
| Fig. 1: Electromagnetic Spectrum. (Source: Wikipedia Commons) |
Cephalometric X-rays are diagnostic radiographs of the lateral skull. They are primarily used in orthodontic treatment planning and by otolaryngologists (ear, nose and throat specialists). Orthodontists use them to visualization the teeth, jawbone, soft tissues, and the nasal and sinus passages. Since the majority of orthodontic patients are children and adolescents, the use of cephalometric X-ray, and the ionizing radiation it generates, has raised health concerns among parents and public health officials. This paper provides an introduction to X-rays, reviews the risks and benefits of cephalometric X-rays, and explores whether better radiographic options are available.
X-rays are one of many forms of electromagnetic radiation (Fig. 1). Their atomic scale wavelength allows them to penetrate the body. As they pass through the body, anatomic structures attenuate the X-rays projecting shadows onto photographic film. Dense structures, such as bone, absorbed most, if not all, of the X-rays the most due to the densely packed bone atoms. Less dense structures, such as the skin or soft tissues, allow the X-rays to pass through with minimal disruption or scatter.
X-rays can be produced by the sudden deceleration of a rapidly moving stream of electrons (generated by a cathode) fired at a positively charged metal target (typically tungsten, the anode) in a vacuum tube. [1] Most dental office X-ray machines produce Bremsstrahlung radiation. Bremsstrahlung radiation is produced in two ways. The first is when electrons directly hit the target materials nucleus producing a single X-ray photon. The second is when the fired electrons pass close to the nucleus, get deflected (but not stopped) and lose some (but not all) of its kinetic energy which is converted into an X-ray photon. The deflected electron continues on its journey and continues to be deflected from additional target nuclei producing many low-level X-ray photons (as opposed to a single photon from a direct nuclear hit). As a result, Bremsstrahlung radiation consists of X-rays of many different energies and wavelengths. [1]
|
||||||||||||||||
| Table 1: Effective dose exposure. [4,5,7,8] (PSP = Photo-stimulatable phosphor; CBCT = Cone-beam computed tomography.) |
Radiation dose is a measure of how much energy is absorbed when someone is exposed to X-rays. There are two commonly used ways to assess radiation dose in dental procedures: skin surface dose and effective dose. Skin surface dose is easier to measure and used in state regulation of X-ray equipment. The effective dose accounts for the various sensitivities of different tissues to radiation over the entire body. Although it is more complicated to calculate, it is a better estimation of the actual radiation-associated risk. [2] The scientific unit for measuring ionizing radiation effective dose is the Sievert (Sv). Dental X-rays are frequently typically reported in micro-Sievert (μSv).
The effective dose of cephalometric X-rays are 5.1 to 5.6 μSv. Table 1 contrasts the effective doses with other common dental X-rays.
X-rays, as one source ionizing radiation, can damage cellular DNA (mutation). If the radiation dose is low and/or it is delivered over a long period (e.g., decades), the risk is substantially lower because the body can repair the DNA damage. [2] However, even at low doses, there remains a risk of long-term effects such as cancer. [3] The risk is higher for children and adolescents because they are more sensitive to radiation exposure and they have a longer lifetime for ill effects to develop. [4] As a result, authoritative bodies have advised the use of the ALARA principle (As Low As Reasonably Achievable) for all dental X-rays including cephalometric. [4]
Since their commercial introduction in 2001, there has been increased use of cone beam CT (CBCT) scans by Orthodontists. [4] Dental CBCT images provide three-dimensional information, which may help with the diagnosis, treatment planning and evaluation of certain dental conditions. [5] While CBCT has some advantages, studies suggest they do not change significantly change orthodontic treatment plans, AND they deliver a higher effective dose of radiation dose (Table 1). [6]
In summary, for routine Orthodontic care CBCT provides minimal advantages, yet increases the patients effective dose exposure of radiation. Therefore, prudent use of cephalometric X-rays should remain the Orthodontists standard of care. However, cephalometric X-rays do emit low levels of ionizing radiation and it remains the Orthodontists responsibility to follow the ALARA Principle.
© Hannah Hales. The author warrants that the work is the author's own and that Stanford University provided no input other than typesetting and referencing guidelines. The author grants permission to copy, distribute and display this work in unaltered form, with attribution to the author, for noncommercial purposes only. All other rights, including commercial rights, are reserved to the author.
[1] P. P. Dendy, Physics for Diagnostic Radiology, 2nd Ed. (Taylor and Francis, 1999), Ch. 2.
[2] Sources and Effects of Ionizing Radiation," (United Nations, 2000).
[3] Health Risks from Exposure to Low Levels of Ionizing Radiation: BEIR VII, Phase 2 (National Academics Press, 2006).
[4] American Dental Association on Scientific Affairs, "The Use of Cone-Beam Computed Tomography in Dentistry," J. Am. Dent. Assoc. 143, 899 (2012).
[5] R. Pauwels et al., "Effective Dose Range for Dental Cone Beam Computed Tomography Scanners," Eur. J. Radiol. 81, 267 (2012).
[6] D. J. Halazonetis, "Cone-Beam Computed Tomography is Not the Imaging Technique of Choice for Comprehensive Orthodontic Assessment," Am. J. Orthod. Dentofacial Orthop. 141, 403 (2012).
[7] J. B. Ludlow, L. E. Davies-Ludlow, and S. C. White, "Patient Risk Related to Common Dental Radiographic Examinations: The Impact of 2007 International Commission on Radiological Protection Recommendations Regarding Dose Calculation," J. Am. Dent. Assoc. 139, 1237 (2008).
[8] "Cone Beam CT for Dental and Maxillofacial Radiology: Evidence Based Guidelines," European Commission, Radiation Protection No. 172, 2012.