 |
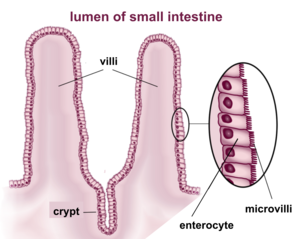
| Fig. 1: Cartoon showing cells in the gastrointestinal system. The stem cells are located within the crypts. (Source: Wikimedia Commons) |
Radiation exposure has serious clinical consequences that depend on the absolute dose of radiation, the dose rate, and any shielding that may have been present and protected specific organs. [1] High levels of radiation exposure lead to acute radiation syndrome (ARS), and previous work has outlined the relationship between radiation dose and clinical symptoms of ARS. [2-4] It is worth noting that hematopoietic syndrome, which involves damage to the immune system and bone marrow and can occur at radiation doses < 1 Gy, is often the main illness observed at lower levels of radiation (0.7-4 Gy) and is the most likely to have lethal effects at high doses of radiation. [5] This report will build on previous work on medical consequences of radiation exposure, but focus primarily on how radiation exposure in the gastrointestinal system leads to acute and chronic clinical symptoms that are important to manage both in the case of accidental radiation exposure and in the application of radiation therapy to treat malignancies.
The gastrointestinal system can be exposed to radiation sufficient to cause clinical symptoms in multiple ways. Large doses of whole-body radiation primarily occur following accidents, many of which occur in the industrial and medical sectors. [6] Exposure of the gastrointestinal system to radiation sufficient to cause clinical symptoms also occurs during radiation therapy for abdominal and pelvic malignancies. [6] In the later case, shielding is used to protect sensitive organs when possible, but, depending on the targets of the therapy, the intestines are often exposed to high doses of radiation. [6]
The clinical consequences of radiation exposure on the gastrointestinal system are largely dose dependent. In patients exposed to whole-body radiation, doses less than 1.5 Gy typically cause nausea, vomiting, and gastric atony. [1,7] More severe symptoms develop in individuals exposed to radiation doses between 5 and 12 Gy. [1] In these patients, loss of intestinal crypt cells and breakdown of the mucosal barrier leads to abdominal pain, nausea, vomiting, diarrhea, and gastrointestinal bleeding. [1] These gastrointestinal symptoms can combine with hematologic complications to accelerate the lethal effects of radiation exposure relative to what occurs with damage to only the hematopoietic system. Such combinatorial effects include an increased likelihood of anemia due to both blood cell loss and gastrointestinal bleeding and an increased likelihood of infection and sepsis due to impaired gastrointestinal barrier function enabling bacterial invasion into the bloodstream of patients with radiation-induced immunosuppression. [1]
Clinical symptoms can also result from radiation exposure specific to the gastrointestinal system, which most commonly occurs in radiation therapy for pelvic and abdominal malignancies. [8] In patients receiving upper abdominal radiation, 50% experience nausea, vomiting, dyspepsia, and abdominal pain, and chronic symptoms can include ulceration and, rarely, gastric wall fibrosis and outlet obstruction. [8] Patients with intestinal radiation exposure often experience nausea, vomiting, diarrhea, and abdominal pain, and, in severe cases, can develop fistulas or intestinal obstructions. [8] Additionally, patients exposed to radiation treatment have been reported to have increased risk of developing additional cancers in the future. [8,9] In patients receiving therapeutic radiation for malignancies, these chronic complications can be life threatening and may limit the therapeutic radiation dose a patient can receive.
Rapidly dividing cells are typically more affected by radiation exposure than resting cells. As a result, the hematopoietic and gastrointestinal systems are some of the most susceptible to radiation damage. In the gastrointestinal system, there are two hypotheses that are commonly employed to explain how radiation effects the gastrointestinal system. Initially, radiation exposure was believed to cause symptoms by directly triggering apoptosis of stem cells located in the intestinal crypts (Fig. 1). [8] When the stem cells are lost, the cells that are shed into the intestinal lumen can no longer be replaced, which can lead to loss of intestinal villi and impaired function. More recently, a second explanation was proposed that suggested that damage to the crypts occurs secondary to endothelial cell damage. This was supported by experiments in mice demonstrating that radiation induced damage to endothelial cells may be the primary driver of intestinal stem cell dysfunction and apoptosis. [8,10] However, subsequent studies have challenged this result and it remains unclear what role this plays in the pathophysiology of gastrointestinal radiation injury. [8]
© Winston Becker. The author warrants that the work is the author's own and that Stanford University provided no input other than typesetting and referencing guidelines. The author grants permission to copy, distribute and display this work in unaltered form, with attribution to the author, for noncommercial purposes only. All other rights, including commercial rights, are reserved to the author.
[1] M. López and M. Martin, "Medical Management of the Acute Radiation Syndrome," Rep. Pract. Oncol. Radiother. 16, 138 (2011).
[2] M. Bae, "Acute Radiation Syndrome," Physics 241, Stanford University, Winter 2017.
[3] J. Lee, "Acute Radiation Syndrome," Physics 241, Stanford University, Winter 2012.
[4] B. Milic, "Symptomatic Development of Acute Radiation Syndrome," Physics 241, Stanford University, Winter 2015.
[5] C. E. Hill-Kayser, E. Glatstein, and Z. A. Tochner, "Radiation Terrorism," in Harrison's Principles of Internal Medicine ed. by D. Kasper et al. (McGraw-Hill,2015).
[6] K. Coeytaux et al., "Reported Radiation Overexposure Accidents Worldwide, 1980-2013: A Systematic Review," PLoS One 10, e0118709 (2015).
[7] I. A. Dubois and R. I. Walker, "Prospects for Management of Gastrointestinal Injury Associated With the Acute Radiation Syndrome," Gastroenterology 95, 500 (1988).
[8] A. K. Shadad et al., "Gastrointestinal Radiation Injury: Symptoms, Risk Factors and Mechanisms," World J. Gastroenterol. 19, 185 (2013).
[9] K. Moon et al., "Cancer Incidence After Localized Therapy for Prostate Cancer," Cancer 107, 991 (2006).
[10] F. Paris et al., "Endothelial Apoptosis as the Primary Lesion Initiating Intestinal Radiation Damage in Mice," Science 293, 293 (2001).