 |
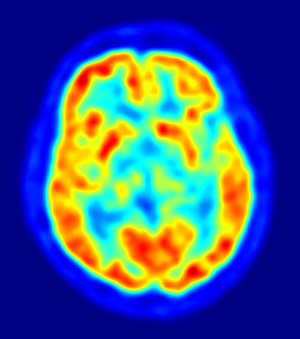
| Fig. 1: Figure 1: Scanned brain image using 18F-FDG. (Source: Wikimedia Commons). |
Positron emission tomography (PET) is an imaging modality that was initially used for the study of brain function through the use of radioisotopes. A lot of work has gone into the development of safe radioisotopes to be injected into humans along with the improvement of the hardware and software comprising a PET scanner. The field has come a long way and currently PET is used for the detection of Alzheimer Disease, to study the effects of stroke and epilepsy, and to locate tumors. [1] Their main clinical use is for oncological imaging of the brain, head, neck, lungs, breasts, colorectal, and prostate. [2] Other uses include the study of pharmacokinectics of drugs used for neurological disorders. [1] As more safe radioisotopes are developed and as improvements are made to PET scanners the uses will continue to increase.
One of the many mysteries of science is how the brain functions. Angelo Morosso is responsible for the idea that brain function is related to blood flow. [3] His claims were revalidated by Charles Roy and Charles Sherrington in 1890, where they concluded that blood flow would be directed to a stimulated portion of the brain according to its function. Autoradiography was used along with gas radiotracers in 1948, initializing the beginning of brain imaging. [1] In 1961 Neils Lassen and David Ingvar used the radiotracer 133Xe to determine the parts of the brain controlling sensory and motor functions. [3]
The first safe radiotracer to be used in humans was 2-deoxyglucose (DG), developed by Louis Sokoloff. It competitively inhibits a portion of the glycolytic pathway, making it a useful molecule to measure the use of glucose in the brain, which directly translates to brain activity. Initially this molecules was radio labeled with 14C but in 1976 Sokoloff along with Dr. Alfred Wolf and Joanna Fowler they synthesized 2-fluoro-2-deoxy-D-glucose (FDG), which is radiolabelled with 18F and is one of the mostly widely used radiotracers today. [1] It has a longer half time (110 minutes) than carbon (20 minutes) and thus allows more flexibility in the measurements. Figure 1 shows a PET image using 18F FDG where the red coloring represents area of high concentration of FDG. Other less commonly used radiolabels in PET are 13N, 15O, and 82Rb, with lifetimes below 10 minutes except for 15O which has a lifetime comparable to 18F. [4]
The scintiscanner was the first instrument used to create images for the detection of radioactivity within the body. It was invented in 1949 by Benedict Cassen and would tap to create dots in a paper; later improved in 1956 by Dr. David Kuhl where the paper was replaced by a radioisotope emission glow lamp (photorecorder) that produced images on X-ray film with a higher resolution. [1,3] The Anger scintillation camera was made in 1957 by Hal O. Anger, which became an essential component for nuclear medicine. [1]
In the 1950s Neurosurgeon William Sweet and physicist Gordon Brownell developed the predecessor to the PET imager in the Massachusetts General Hospital using sodium iodide (NaI) as the detector. [3] By the 1970s the technology had improved to contain 24 NaI detectors that had capabilities for attenuation correction and filtered backprojection. Alternatives to the NaI detector were necessary since this detector had high scatter and low density which limited its resolution and efficiency, respectively. An alternative was found in the 1980s in bismuth germanite (BGO) which had a high density and a similar decay constant as NaI. With this crystal the first commercially available PET scanner was made. The 1990s saw the technology improved by using 24-ring geometry with 11,520 BGO crystals and a spatial resolution of 2.9 mm. Another detector discovered was lutetium oxy-orthosilicate (LSO) which has an even higher density and a faster decay time than BGO and therefore has a higher sensitivity and lower random events, resulting in a resolution of 2.5 mm and 3D imaging. [1]
A strong effort has been under place to improve PET technology. The search for better detectors and different radiotracers has and continue to be explored. A combination of CT and PET is a common technique used due to CT's high anatomical detail. MRI also has that attribute though is not as commonly used in conjunction with PET. [1] The next step would be to combine all three technologies for a better detection of disease and monitoring of neurological and cancer drug treatments.
© Gabriela Bernal. The author grants permission to copy, distribute and display this work in unaltered form, with attribution to the author, for noncommercial purposes only. All other rights, including commercial rights, are reserved to the author.
[1] T. Abraham and J. Feng, "Evolution of Brain Imaging Instrumentation," Semin. Nucl. Med. 41, 202, (2011).
[2] C. Schiepers, C. K. Hoh, "FDG-PET Imaging in Oncology," in Diagnostic Nuclear Medicine, ed. by A. L. Baert, K. Cartor and C. Schiepers, (Springer, 2006), p. 185.
[3] L. H. Portnow, D. E. vaillancourt, and M. S. Okun, "The History of Cerebral PET Scanning," Neurology 80, 952, (2013).
[4] F. A. Mettler and M. J. Guiberteau, Essentials of Nuclear Medicine Imaging, 6th Ed., (Saunders,2012), p. 1.